How to manage type 2 diabetes if you’re over 60
Although type 2 diabetes (T2D) is technically the same in everyone (beta-cell dysfunction and insulin resistance), its presentation can differ slightly between people, and this is where “personalised” nutrition can be useful.
T2D in older age groups is one of these cases.
Weight loss?
People with T2D who are over the age of 60 years typically have lower BMIs compared to younger age-groups. While some people may benefit from a little bit of weight loss, more marked or dramatic weight loss is not always appropriate. In fact, many patients are see worry about losing too much weight and not feeling so good.
We of course need to remember that BMI isn’t everything. In fact, many people can have a normal BMI but significant internal fat. A larger waist circumference (and generally gathering weight around the middle) is a good surrogate of this.
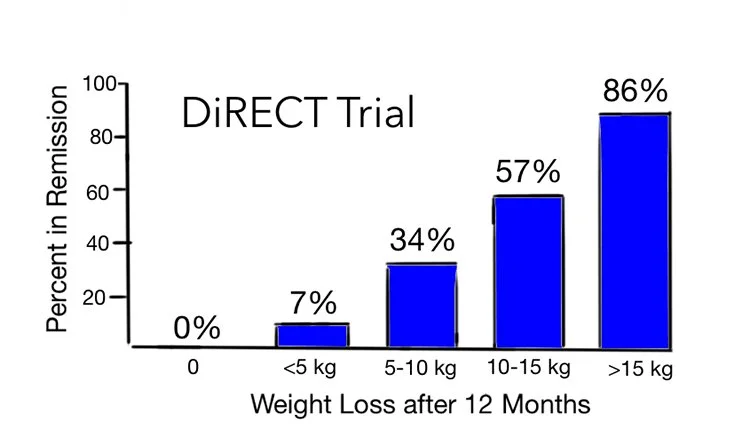
This is especially relevant when we come to remission (Blood glucose at non-diabetic levels without needing diabetes medications). Remission of diabetes is something many, many patients want to achieve. At the present time, the best evidence we have is that weight loss is the primary driver of remission. (The figure below is quite clear on this). We think that weight loss helps a person reduce ectopic fat, like liver fat - and that this plays a big role in helping the pancreas work better.
Lean ME et al. Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. Lancet. 2018;391(10120):541-551.
In fact, I have seen patients in my clinic who have become incredibly thin - sometimes to the point of appearing very frail - in their quest to achieve remission, because they are desperate to achieve “0% fat in their liver”.
However, the good news is that there are ways to lower glucose - and - “internal” fat without weight loss. Here are my top three tips.
1) Increase protein and decrease carbohydrate.
This is a very effective way of lowering glucose substantially (2-4mmol/L!) without weight loss, and also helps lower liver fat too!
Protein is very effective because it breaks down into amino acids, and the amino acids then stimulate the pancreas to produce more insulin at meals. What is especially cool is that this works even if people have had T2D for a long time. You may have heard that remission is less likely in people who have had T2D for more than 6 years. We think this is because the pancreas becomes less sensitive to glucose (carbohydrate). So when you eat any carbohydrate - and your blood glucose goes up - your pancreas can’t recognise the increase in glucose, and so doesn’t produce any insulin. It’s like the pancreas become blind to insulin! But the pancreas does remain sensitive to amino acids!
A diet with about 30% of calories from protein and 20-40% of calories from carbohydrate has been shown in multiple trials - including my own - to lower glucose.
This diet is also consistent with recommendations that older adults need a higher intake of protein (1.2g/kg) regardless of whether they have T2D or not.
Note that people with kidney disease should check with a doctor before following this diet. Increased protein is not recommended in people with advanced stages of chronic kidney disease (CKD).
Download this diet sheet for practical tips on how to put this diet into practice.
2) Do more exercise, especially resistance-type training.
We lose muscle mass and strength as we age, and this accelerates after around the age of 60 years. The no-brainer countermeasure to this is resistance exercise! It doesn’t need to be super heavy. Try to resistance train at least twice a week, lifting challenging loads that help build strength. When lifting a weight becomes too easy, add more! You don’t need a personal trainer to do this, but sometimes having someone to show you the ropes for one session can be useful so you know what to do.
All any any exercise also helps improve insulin sensitivity and reduce ectopic fat - even without weight loss!
3) Have more whole plant foods which contain fermentable or viscous fibres
Viscous/fermentable fibres are a type of carbohydrate which are not digested and absorbed in the upper gastrointestinal tract like most carbohydrates. Instead they pass intact to the colon where they are fermented (digested!) by the gut bacteria there. Products of this “colonic” fermentation include the short chain fatty acids (SCFAs) which seem to help regulate fat metabolism,. For example, studies of fermentable or viscous fibres show they increase fat oxidation and improve insulin sensitivity. Some studies suggest they can lower liver fat as well!
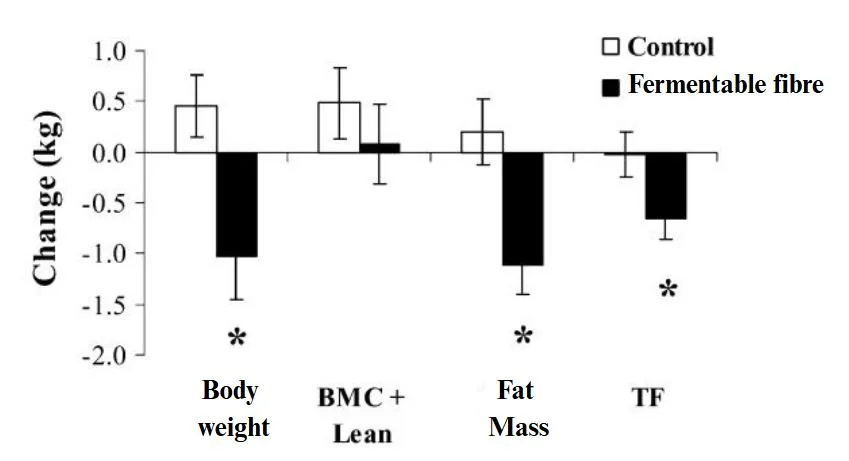
Take a look at this study. They gave a fermentable fibre (oligofructose (OFS)) to people during a weight loss intervention, while a control group got a non-fermentable fibre (cellulose). The OFS lost more of their weight as fat than the control group.
Parnell JA, Reimer RA. Weight loss during oligofructose supplementation is associated with decreased ghrelin and increased peptide YY in overweight and obese adults. Am J Clin Nutr. 2009 Jun;89(6):1751-9. doi: 10.3945/ajcn.2009.27465.
There is also some cool data coming through the ultraprocessed food (UPF) research that suggests that even if a nearly entirely UPF diet doesn’t cause people to gain weight, it negatively impacts body composition. This data I am talking about is the interim output from a new study - but I think it is pretty alarming if bourne out in the final results. I think the change in body composition is due to the lack of whole - fermentable or viscous - fibre in the UPF diet.
So - having a decent amount of these fibres in the diet is important because it probably helps us limit fat deposition generally, but more specifically in the places we want it least!
Improving body composition also helps improve T2D control!
See this diet sheet for foods to add in your diet (the good news is some of them are high protein too!) to ensure you are getting these beneficial fibres in.